Scoliosis: A More Common Spinal Condition Than You Think
Dr. Teresa Rodríguez del Real
Have you noticed your child has one shoulder slightly higher than the other, or perhaps some asymmetry in their back? It might seem like a minor postural habit, but these signs can be the first clues of a spinal curve or deformity.
In Spain, it is estimated that between 2% and 3% of young people aged 10 to 16 suffer from what is known as adolescent idiopathic scoliosis—affecting tens of thousands of teenagers. Many of these cases are mild, asymptomatic, and go unnoticed. However, if not detected early, they can progress.
This is where an in-home orthopedic service becomes invaluable. It allows for a specialized evaluation in a comfortable, familiar environment—ideal for families with children or individuals with reduced mobility—ensuring early detection without the stress of a clinical setting.
What is Scoliosis? Types and Classifications
Scoliosis is a structural deformity of the spine that often includes vertebral rotation. Instead of following a straight vertical line, the spine develops a “C” or “S” shape. This curvature is not merely a lateral lean; it can impact posture, balance, and, in severe cases, respiratory function or overall mobility.
Classification by Age of Onset
Understanding when scoliosis first appears is crucial for prognosis and treatment planning:
Infantile Scoliosis (Birth to 3 years): The rarest form. While prevalence is low, active monitoring is essential as some cases resolve spontaneously, while others require early intervention.
Juvenile Scoliosis (3 to 10 years): Since the skeleton is still growing rapidly, the risk of curve progression is high. Treatment focuses on control through observation, bracing, or, in severe cases, surgery.
Adolescent Idiopathic Scoliosis (AIS) (10 years and older): The most common form. It often surfaces during the pubertal growth spurt. Management depends on the degree of the curve and the patient’s remaining growth potential.
Adult Scoliosis (Post-skeletal maturity): This involves two scenarios:
Progression of pre-existing scoliosis: A curve from youth that worsens due to degenerative changes (arthritis or disc wear).
Degenerative (De Novo) Scoliosis: Developing after age 40 or 50, primarily caused by asymmetrical degeneration of intervertebral discs and facet joints.
Note on Modern Classification: Today, specialists often simplify this into Early-Onset Scoliosis (before age 10) and Late-Onset Scoliosis (after age 10). Early-onset cases, particularly in children under 5, require closer attention as they can affect cardiopulmonary development.
Warning Signs: When to Suspect Scoliosis
While some cases are obvious, others are subtle. Early detection is the key to avoiding invasive treatments. Parents should look for the following signs at home:
Physical and Postural Red Flags
Asymmetric Shoulders or Hips: One shoulder appearing higher than the other or an uneven hip line.
Body Imbalance: The head may appear off-center or the torso may seem to lean to one side.
Waist Irregularity: An uneven waistline or skin folds that are deeper on one side.
Prominent Shoulder Blades: One scapula sticking out more or appearing higher than the other.
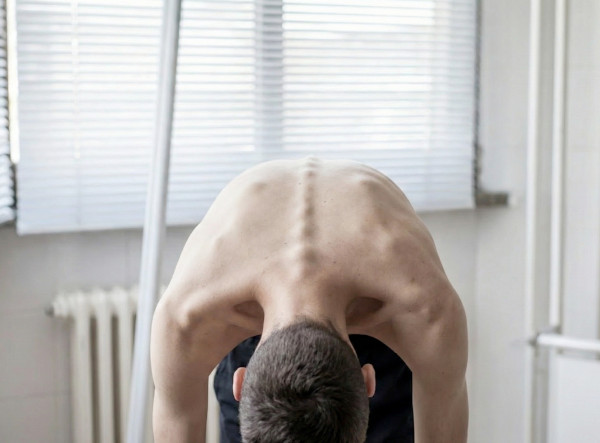
The Adams Forward Bend Test
This is a simple and reliable screening tool you can perform at home:
The Action: Have the person lean forward slowly with arms hanging freely and palms together (as if diving), keeping the knees straight.
What to Look For: In a scoliotic spine, this position reveals a rib hump (a prominence in the upper or lower back) caused by the rotation of the vertebrae.
In most instances, scoliosis is painless. This lack of symptoms is why regular postural observation and professional consultations are vital.
Why Early Diagnosis and Follow-up are Critical
Adolescence is a high-risk period because rapid growth can cause a mild curve to progress significantly in a short time. Depending on the case, a check-up every 6 to 12 months is recommended.
Early diagnosis allows for conservative treatments, such as specialized bracing, which can prevent the curvature from reaching a stage where surgery becomes the only option.
The Value of an In-Home Orthopedic Specialist
Our home-visit traumatology service offers distinct clinical advantages:
Natural Environment: The specialist can observe the patient’s real-life ergonomics—how they sit, move, and study—and tailor recommendations accordingly.
Brace Monitoring: For patients using a brace (orthosis), adjustments and progress checks can be done comfortably at home.
Stress Reduction: Avoiding hospital environments reduces anxiety for children and adolescents, fostering better cooperation and consistency with treatment.
Beyond Treatment: Prevention and Daily Management
Maintaining core strength and healthy postural habits is essential at every stage of life.
For Children and Adolescents:
Postural Education: Encourage sitting with the back fully supported and feet flat on the floor.
Backpack Safety: The weight should never exceed 10-15% of the child’s body weight. Use wide, padded straps on both shoulders and a waist belt if possible.
Comprehensive Physical Activity: Focus on “symmetrical” sports like swimming or dance to develop balanced muscle tone in the trunk and paraspinal muscles.
For Adults:
Core Strengthening: Low-impact exercises like Pilates, swimming, or brisk walking create a “natural muscular brace” that protects the spine.
Weight Management: Excess abdominal weight shifts the center of gravity, increasing lumbar strain and worsening spinal curves.
Digital Ergonomics: Hold mobile devices at eye level to avoid “text neck” and use ergonomic chairs during work hours, taking stretching breaks every 45 minutes.
Sleep Tips:
Choose a medium-firm mattress and a pillow that keeps the head aligned with the spine. For those with a “C-shaped” curve, specialists sometimes suggest sleeping on the side of the concavity (the “hollow” side) to help open the curve, though this should always be confirmed by your specialist.
Take Action Today
Do you or your child show any of these signs? Do not wait for the condition to progress. Request a specialized in-home evaluation. A professional assessment in the comfort of your home can make all the difference in long-term spinal health. Contact us today for a personalized consultation.

